
Healthcare
Creating machines that can see the information in the images that the human eye cannot
Healthcare focuses on medical imaging technologies for cancer detection and machine learning in personalised care for better living and healthy ageing.
Research leads

Professor Kevin Wells
Professor of AI in Human and Veterinary Healthcare

Dr Lucia Florescu
Lecturer in Medical Imaging

Dr Samaneh Kouchaki
Senior Lecturer in Machine Learning for Healthcare
Overview
The NHS has identified priority medical conditions, such as cancer, sleep disorders, and ageing and dementia. We have been addressing these healthcare challenges in collaboration with key stakeholders in the sector.
Diagnosis and treatment of these health conditions have been enhanced by our medical imaging research. This has been achieved by bringing together techniques drawn from AI, computer vision and machine learning with biomedical physics and simulation. A multidisciplinary approach has been forged, with collaborations across University departments as well as leading research institutions and industrial partners, such as the National Physical Laboratory, Alliance Medical and Elekta.
Professor of Medical Radiation Imaging Philip Evans, says: “In order that our work is useful and relevant to the needs of clinicians and patients alike, we work closely with clinical experts and industry to ensure our work delivers real-world application. Our clinical collaborators provide not only the initial rationale for much of our work, but are also intimately involved in its development, providing expert feedback to optimise clinical impact and utility.”
To help achieve this, collaboration with key stakeholders is crucial. We are working in the UK with the Royal Surrey County Hospital, The Royal Marsden Hospital/The Institute of Cancer Research, St George’s Hospital, Addenbrooke’s Hospital Cambridge, University College London and University Hospitals Birmingham. Internationally, we work with the German Cancer Research Center, Heidelberg, and the MAASTRO clinic in Maastricht.
Using virtual clinical trials for breast cancer screening

We are part of an ongoing collaboration to optimise the use of clinical techniques in breast cancer screening, using the concept of Virtual Clinical Trials (VCT). All new medical technologies need to be tested on humans before being approved for clinical use, but this can take up to five years. Plus, a cancer screening trial requires thousands of potentially healthy participants who will be exposed to X-ray radiation.
Our Centre, in collaboration with Royal Surrey County Hospital, has developed a unique set of validated simulation tools that can generate artificial X-ray images of breast cancer that are indistinguishable from their real-life counterparts. Such simulated images allow the study of the types of cancer, the types of tissue, the types of imaging system and the way the image are produced in a uniquely controlled way. This enables the investigation of specific ‘task-based assessment’ questions which can be answered in a VCT that would be impossible using conventional clinical trials.
Dr Kevin Wells says: “ This collaborative project, involving three UK hospitals, has led to VCTs with no patients, no humans exposed to radiation, and the use of AI to replace human operators. Running a trial can now take days rather than years.”
Internet of Things for better living and healthier ageing

With growing environmental challenges and an ageing population, we need to find effective solutions to make our communities’ infrastructure more sustainable and develop services that provide more efficient healthcare.
We are living in an increasingly interconnected world, in which technology allows us to interact with people, physical objects and devices remotely. Computer systems can gather continuous data from our homes, offices and cities in real-time, while wearable devices enable the collection of personalised activity data, and the ability to interact with users any time and almost anywhere.
The network of interconnected sensors, actuators and network enabled devices known as the Internet of Things (IoT) is growing exponentially. In CVSSP, we are combining these IoT technologies with AI and machine learning algorithms to develop advanced systems which tackle some of the key challenges faced by society such as traffic, waste management, and healthcare.
IoT technologies provide unique opportunities to design and develop services that can use data analytics and machine learning techniques to obtain near real-time intelligence about people’s health and environment, or a city’s resources. However this also brings some major challenges. Gathering sensitive personal data for healthcare applications, for example, brings a range of security and privacy risks. Accessibility is another important consideration.
Professor of Machine Intelligence Payam Barnaghi explains: “Connected communities and smarter solutions should not help create a new digital gap. These essential and beneficial services need to be designed in such a way that they are applicable and accessible to citizens across all demographic groups.”
Supporting people with dementia

Technology Integrated Health Management (TIHM) for dementia – led by Surrey and Borders Partnership NHS Foundation Trust and CVSSP, is an AI and Internet of Things study which harnesses low-cost sensory technologies and machine learning algorithms to support people with dementia living at home.
In the first phase of the study, which involved more than 400 people with dementia and their carers from Surrey and North East Hampshire, participants were remotely monitored using a network of internet-enabled devices installed in their homes in combination with AI algorithms that were developed to alert clinicians when support was needed.
“With our ageing population on the rise, there is an increased need for innovative projects to ensure that all their care needs are met. In TIHM, machine learning and Internet of Things technologies help to provide actionable-information to clinicians and users in remote monitoring and care for dementia, “ explains Dr Shirin Enshaeifar.
TIHM for dementia has been recognised with a number of high profile awards including the HSJ 2018 Award for Improving Care with Technology and ‘Best Mental Health Initiative’ in the 2017 EHI Awards.
Improving lives through medical imaging
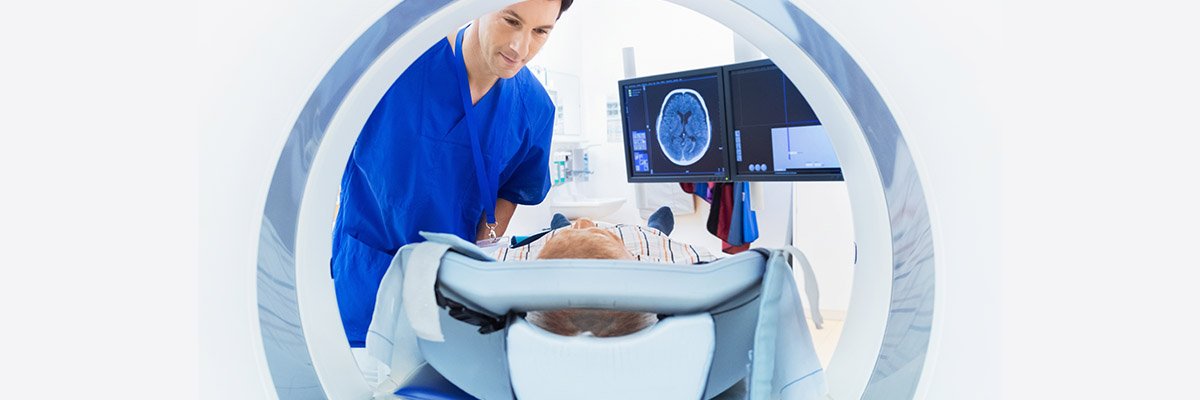
In modern cancer therapy, medical imaging plays an essential part in allowing the clinical team to detect the location and extent of a tumour. Within CVSSP we are developing methods to train the computer to see information in the images that the human eye cannot.
Our medical imaging experts are developing new methods for both capturing better images, and analysing repeating patterns more effectively, which is opening the door to more personalised treatments.
One of these pioneering techniques involves reconstructing images from the raw data acquired by the scanner, utilising a range of methods including optical tomography, computed tomography, magnetic resonance imaging (MRI), positron emission tomography, ultrasound and imaging with a proton radiotherapy beam.
Our research also focuses on uncovering the information hidden in medical images, which is vital for accurate diagnosis of the type and aggressiveness of the cancer. This hidden information is contained in features such as the ‘texture’ or fine grain structure of the images, and the mathematical properties of the intensity values contained in the images.
“Using these innovative approaches could enable doctors to determine the position of the tumour more accurately, which would mean that radiation could be directed more precisely, allowing treatment to be adapted to the individual”, explains Professor of Medical Radiation Imaging Philip Evans.
Our methodology is now being evaluated in a study of 300 lung cancer patients who are being treated with both radiotherapy and surgery. With lung cancer having been identified as a ‘cancer of unmet need’, with a poorer outcome than many other common cancers, our research has the potential to make a tangible difference to many lives.
PhD student develops innovative image analysis technique
Dr Sheaka Alobaidli, who studied for a PhD in medical physics in CVSSP, is now Head of Radiotherapy Physics at the Kuwait Cancer Control Centre.
She explains: “After my masters in medical physics, I was very interested in cancer imaging, and I realised that doing my PhD in CVSSP would be a great opportunity. During my PhD I got the chance to work with experts from the field of signal processing, medical physics, radiology and oncology which enriched my knowledge and allowed me to grow as a researcher.”
Dr Alobaidli’s PhD project on ‘functional imaging and texture analysis in radiotherapy planning’ was a joint project with the Royal Surrey County Hospital NHS and Guildford Diagnostic Imaging.
“As a PhD student, Sheaka developed an innovative method of using image analysis to help plan radiotherapy treatment for lung cancer. By working out the regions of the tumour that are going to be less or more sensitive to radiation, or more likely to have cancer cells, this could lead to far more effective, personalised treatments.” – Professor Phil Evans (PhD supervisor).
Research projects
- Quantitative radiomics in lung cancer treatment planning and analysis
- Quantify metabolic activity using hyperpolarized [1-13C] and/or 1H MR Spectroscopy
- Cancer detection and characterization based on multi-parametric MRI
- Polarisation-Sensitive Optical Tomography
- Machine learning and virtual clinical trials in digital mammography
- Tomographic imaging for proton beam radiotherapy
- Dose and image guided brachytherapy for gynaecological and prostate cancer treatment
- Non-contact optical imaging for medical imaging acquisition
- Standardisation of imaging in radiology for applications including image guided radiotherapy and texture analysis.
- Cancer Research UK Programme (2013-2018) “OPTIMAM2: Optimisation of breast cancer detection using digital X-ray technology” – Wells
- Wellcome Fellowship (2017-2021) “Optical characterisation of epithelial tissue function and metabolism for early cancer diagnosis and treatment monitoring” – Florescu
- EPSRC project: (2018-2019) “Novel image reconstruction techniques with application to proton radiotherapy for optimisation of cancer treatment” – Dikaios.






