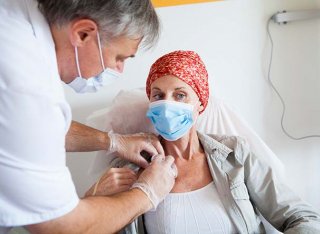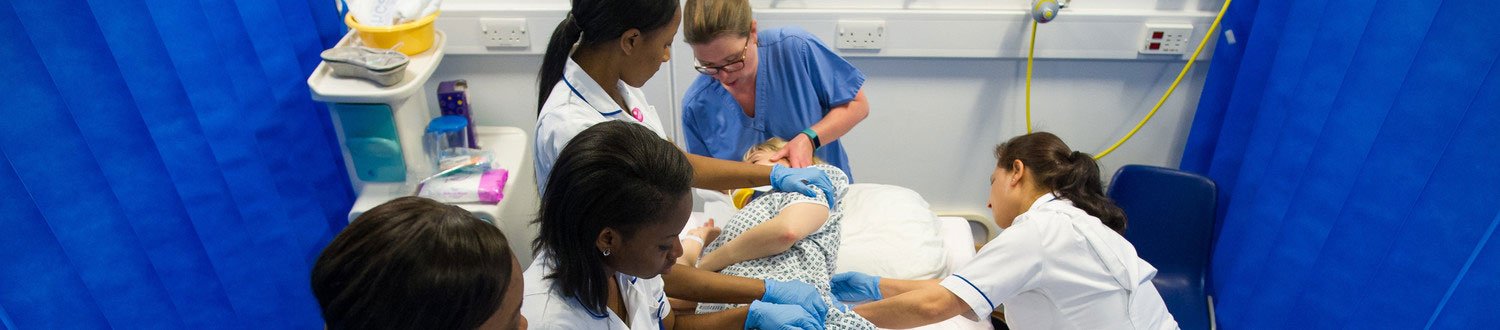


Cancer Care Expert Group
Our mission is to improve cancer care for all. We work with experts from a diverse range of disciplines, including technology, science, engineering and psychology. We work alongside NHS professionals, Government, patients and their families, from the very young, to the very old. When we work together, we create innovative ways of being diagnosed quicker and living well, with and beyond cancer. Our work helps optimise cancer outcomes and impacts positively on experiences of care.
Research interests
Evidence shows that people with cancer have unmet needs, particularly at the point of diagnosis, end of treatment and longer term. Whilst some people feel well, others are struggling with the consequences of cancer treatment, creating a burden of illness that impacts on quality of life, patient outcomes and family life. Early diagnosis is considered a cornerstone of improving cancer survival- and is importantly related to improved patient experience and quality of life.
Our work focuses on changing the way we diagnose and support people with cancer – and families managing cancer – in order to meet increasing demands and care needs. We work across the age span and disease course - from diagnosis to survivorship and palliative care.
Research areas
- Early diagnosis
- Inequalities in cancer outcomes (individually and intersectionally)
- Cancer as a chronic condition
- Influence of cancer treatment on people, informal carers, parents, siblings and other family members. Specific interests include:
- Symptom assessment and management
- Psychological support needs
- Decision-making
- Multi-morbidity
- Survivorship
- End-of-life care.
- Patient reported outcome and experience measures
- Optimising teamwork and patient care
- Digital health/connected health, supportive technologies and web-based programmes to support mental and physical health for people with cancer
- Improving access and equity in cancer care
- Cancer care system policy.
Research methodologies
- Participant co-design
- Mixed methods
- Development and evaluation of complex interventions
- Film technologies
- Creative arts based approaches.
- Research Priority Setting Partnerships
- Questionnaire design and validation approaches
- Data linkage, statistical and machine learning
- Intersectionality and transformative methods.
Areas of interest for doctoral study
We welcome approaches from people wishing to undertake postgraduate research with us. We particularly welcome enquiries in the following areas:
- Prevention and early diagnosis
- Supportive care and innovations
- Cancer in children, teenagers and young adults
- Digital health.
Please contact Freda Mold (freda.mold@surrey.ac.uk) and Jenny Harris (jen.harris@surrey.ac.uk), our postgraduate research directors, if you are considering postgraduate research.
Our studies
- Understanding and addressing inequities in cancer care for people with a learning disability
- Cancer Research UK - Identifying, understanding and addressing inequalities in cancer treatment. 2025- 2031 (PI Rob Kerrison with Katriina Whitaker, Natalie Gil, Tanya Perchyk and external collaborators)
- Children’s Cancer and Leukaemia Group. Getting the ending right: feeling prepared to move into survivorship care when active treatment finishes. Co-PIs Susie Aldiss and Faith Gibson.
- Validation of canine oncology-proxy reported outcome measure to support symptom management and quality of life in dogs undergoing chemotherapy
- Breast Cancer Now - Inequalities in routes to diagnosis, diagnostic intervals, and pre-treatment intervals, for breast cancer, before and after the COVID-19 pandemic: a retrospective analysis of national data. 2023 - 2025 (PI Rob Kerrison with Katriina Whitaker, Agnieszka Lemanska and external co-apps)
- NIHR RfPB-Does Personalised Stratified Follow-Up (PSFU) meet the health and wellbeing needs of people from under-served groups who have completed treatment for breast cancer? A qualitative study (Co-PIs K Sutton & J Armes). 21 months, starting 01/09/24.
- Morris Animal Foundation- Validation of Canine Oncology-Proxy Reported Outcome Measure (CO-PROM) to support symptom management and quality of life in dogs undergoing chemotherapy. (PI J Harris) (24-month project)
- NIHR Policy Research Unit in Cancer Awareness, Screening and Early Diagnosis (2024-2029, Katriina Whitaker and Rob Kerrison).
- NIHR HSDR - Improving uptake, experience and implementation of interpreting services in primary care: a mixed methods study with South Asian communities in. England. (2022-2025, PI Katriina Whitaker with Sabine Braun, Graham Hieke and external co-apps)
- James Lind Alliance Children’s Cancer Priority Setting Partnership
- Development and validation of a blood cancer awareness measure
- How is cancer care best provided to patients in English prisons? Assessing the disease burden in the prison population, experiences of diagnosis, treatment and support, and of receiving and providing cancer care
- University Global Partnership Network: Cancer INequalities Collaboration (UGPN CINC)
- Creative methods of engaging children and young people with cancer in research (Susie Aldiss; supervised by Faith Gibson and Anna Cox)
- Adverse events and quality of life in patients with advanced melanoma being treated with immunotherapies (Alexandra Pritchard; supervised by Jo Armes and Jenny Harris)
- The psychosocial needs of siblings when a brother or sister is diagnosed with cancer (Zoe Polly; supervised by Faith Gibson and Anna Cox)
- Understanding breast cancer screening uptake among women of Black African descent in the UK- Individual and socio-cultural factors (Anietie Aliu; supervised by Afrodita Marcu and Robert Kerrison).
- How, why, for whom and in which contexts does telemedicine work to meet the routine follow-up consultation needs of people with malignant and non-malignant haemato-oncological disorders? (Michelle Kenyon; supervised by Emma Ream and Cath Taylor).
- Mapping factors into breast cancer inequities and depicting pathways to action to close the care equity gap: A transformative and intersectional mixed methods study. (Mar Estupiñán Fdez. de Mesa; supervised by Katriina Whitaker, Emma Ream and Afrodita Marcu)
- Improving supportive care during immunotherapy: co-design of a patient reported outcome measure to assess adverse events in people with renal and melanoma cancers (Alexandra Pritchard; supervised by Jo Armes and Jenny Harris).
- Adaptation and pilot testing of the Registered Nursing Forecasting (RN4CAST) nurse survey for use in the ambulatory chemotherapy setting (Zhuming Bao; supervised by Jo Armes and Jenny Harris).
- Improving predictive validity of tumour markers in pancreatic cancer: Developing and validating predictive models using a large United Kingdom primary care database (Claire Price; supervised by Agnieszka Lemanska, Nadia Smith (National Physics Laboratory) and Debbie Cooke).
- Data-driven solutions to improving pancreatic cancer diagnosis. Developing and piloting a primary care intervention (Hugh Claridge, supervised by Agnieszka Lemanska, Spencer Thomas),
- Data-driven solutions to address healthcare inequalities of prostate cancer in the United Kingdom using routinely collected primary care data (Gayasha Somathilake; supervised by Agnieszka Lemanska, Sotiris Moschoiyannis and Elizabeth Ford (Brighton and Sussex Medical School)
- Improving early cancer diagnosis for people with learning disabilities. (Natalie Gil; supervised by Robert Kerrison, Anna Cox and Katriina Whitaker)
- Investigating the influence of early diagnosis on psychological adjustment in cancer survivorship (Laura Boswell; supervised by Katriina Whitaker, Jenny Harris, Jo Armes, and Georgia Black (Queen Mary University of London)
Publication highlights
Aliu, E. A., Kerrison, R.S., Marcu, A. 2025. A Systematic Review of Barriers to Breast Cancer Screening, and of Interventions Designed to Increase Participation, Among Women of Black African and Black Caribbean Descent in the UK. Psycho-Oncology. https://doi.org/10.1002/pon.70093
Bryan, G., Gibson, F., Aldiss, S. 2025. The Child's Voice in Adult-Led Healthcare Research: One Child Doesn't Fit All!. Comprehensive Child and Adolescent Nursing, 1–10. Advance online publication. https://doi.org/10.1080/24694193.2025.2478046
Davies, E.A, Lüchtenborg, M., Maree Hunter, R., Visser, R., Huynh, J., Pow, R., Plugge, E., Taylor, R.M., Armes, J. Cancer in English prisons: a mixed-methods study of diagnosis, treatment, care costs and patient and staff experiences.2025. Health Soc Care Deliv Res. 2025 Feb;13(3):1-51. doi: 10.3310/HYRT9622. PMID: 39982760.
Estupiñán Fdez de Mesa, M., Ferguson, M., Green, S., Marcu, A., Ream, E., Whitaker, K.L. 2025. Applying the intersectionality lens to understand minority ethnic women’s experiences of the breast cancer care pathway in England: A qualitative interview study. Psycho-oncology, 34(2)e70092, doi: 10.1002/pon.70092.
Gil, N.M. Merriel, S.W. Sailem, H. Cummins, G. Finn, E. Kerrison, R.S. 2025. Patient acceptability of an ingestible sampling and imaging capsule (Samplecam) for bowel surveillance and early detection of colorectal cancer among Lynch Syndrome patients: a focus group study. Frontiers in Cancer Control and Society. doi: 10.3389/fcacs.2025.1568786
Harris, J., Fournier, Q., Sutton, K., Armes, J., Ream, E., Bacon, N. A rapid state-of the-art review of client-reported outcomes measures used to assess dogs’ clinical signs and quality of life during chemotherapy. BMC Vet Res. 2025 Feb 18;21(1):74. doi: 10.1186/s12917-025-04522-4.
Kerrison, R.S. Gil, N. Stoffel, S. Hirst, Y. Whitaker, K.L. Rees, C. Duffy, S. and Von Wagner C., 2025. Effectiveness of behavior change techniques to address barriers to follow-up colonoscopy: results from an online survey and randomized factorial experiment. Annals of Behavioral medicine. https://doi.org/10.1093/abm/kaae083
Marcu, A., Ream, E., Poole, K., Armes, J., Gibson, F., Whittaker, L., Harris, J. 2025. Symptom appraisal and help-seeking before a cancer diagnosis during pregnancy: a qualitative study. British Journal of General Practice. https://doi.org/10.3399/BJGP.2024.0208
Postma, L., Gibson, F., Jagt, J. Z., Aussems, K., Barrett, H., Luchtenberg, M., Schoemaker, C. G., Temple, R. K., Aldiss, S. 2025. Exploring Experiences and Designing Guidance for Involving and Engaging Children and Young People in James Lind Alliance Priority Setting Partnerships. Health Expectations, 28(2), e70195. https://doi.org/10.1111/hex.70195
Somathilake, G., Ford, E., Armes, J., Moschoyiannis, S., Collins, M., Francsics, P., Lemanska A. 2025. Evaluating the quality of prostate cancer diagnosis recording in CPRD GOLD and CPRD Aurum primary care databases for observational research: A study using linked English electronic health records. Cancer Epidemiol ;94:102715. doi: 10.1016/j.canep.2024.102715.
Sutton, K., Armes, J., Michael, A., Skene, S., Mansi, J. (2025)The Perceptions of Patients, Carers and Clinicians Relating to SACT Decision-Making in Older People With Cancer: Qualitative Findings From the Electronic Frailty Index (eFI) in Cancer Study, In: European Journal of Cancer Care: DOI: 10.1155/ecc/4399728
Armes, J., Visser, R., Lüchtenborg, M., Huynh, J., Wheatcroft, S., Anthony, X., Barber, A.E., Plugge, E., Taylor, R.M., Hunter, R.M. and Davies, E.A., 2024. Cancer in prison: barriers and enablers to diagnosis and treatment. eClinicalMedicine. https://doi.org/10.1016/j.eclinm.2024.102540
Bao, Z., Harris, J., Lavender, V., Anne Marie Rafferty and Armes, J. (2024). Understanding Nurses' Role in Systemic Anti-cancer Therapy Day Unit: A Qualitative Study: Seminars in Oncology Nursing, pp.151720–151720. doi:https://doi.org/10.1016/j.soncn.2024.151720.
Baxter, M.A., Denholm, M., Kingdon, S.J., ...& Harris, J. 2024. CAnceR IN PreGnancy (CARING)–a retrospective study of cancer diagnosed during pregnancy in the United Kingdom. British Journal of Cancer, 130(8), pp.1261-1268.
Clothier, Z., Armes, J., Kehinde, A., Mumford, V., Upshon, K., Williamson, C., MacAthur, R., Stevenson, R., Otter, S., Teoh, M., Harris, J. (2024)Patient reported experience measures to assess psychosocial cancer care: A rapid review of current instruments, In: Measurement and Evaluations in Cancer Care2100007 Elsevier Inc
Cockle-Hearne J, Groothuizen JE, Ream E, Helping patients prepare their dependent children for parental death: mixed-methods evaluation of a codeveloped training programme for palliative and allied healthcare professionals in the UK BMJ Open 2024;14:e081775, https://doi.org/10.1136/bmjopen-2023-081775
Estupiñán Fdez. de Mesa, M., Marcu, A., Ream, E., & Whitaker, K. L. (2024). Understanding and tackling cancer inequities: What opportunities does intersectionality offer researchers, policymakers, and providers? A scoping review. Journal of Psychosocial Oncology, 1–28, https://doi.org/10.1080/07347332.2024.2361642
Estupiñán Fdez. de Mesa, M., Marcu, A., Ream, E., Whitaker, K.L. 2024. Using the Candidacy Framework to understand individual, interpersonal, and system level factors driving inequities in women with breast cancer: a cross-sectional study. BJC Reports 2, 83 (2024). https://doi.org/10.1038/s44276-024-00103-4
Estupiñán Fdez. de Mesa, M., Marcu, A., Ream, E., Whitaker, K.L. (2024). Socioeconomic inequities in care experienced by women with breast cancer in England: An intersectional cross-sectional study. European Journal of Oncology Nursing,72, 102648, https://doi.org/10.1016/j.ejon.2024.102648.
Hunter, R.M., Huynh, J., Lüchtenborg, M., Armes, J., Plugge, E., Taylor, R.M., Visser, R. and Davies, E.A., 2024. Does the cost of cancer care for people in prison differ from those in the general population? Analysis of matched English cancer registry and hospital records. eClinicalMedicine. https://doi.org/10.1016/j.eclinm.2024.102575
Ivany, E., Dunn,E., Cannon, N., Lavendar, V. (2024). A compassionate communication skills training course for staff working in cancer services. Cancer Nursing Practice. Vol 23, Issue 4. https://doi.org/10.7748/cnp.2024.e1867
Jeffs, E., Ream, E., Taylor, C. et al. Evidence for the clinical effectiveness of decongestive lymphoedema treatment for breast cancer–related arm lymphoedema, a systematic review. Support Care Cancer32, 568 (2024). https://doi.org/10.1007/s00520-024-08759-x
Lemanska, A., Andrews, C., Fisher, L., Bacon, S., Mehrkar, A., Inglesby, P., Davy, S., Goldacre, B., MacKenna, B., The OpenSAFELY Collaborative, Walker, A.J. (2024) During the COVID-19 pandemic 20 000 prostate cancer diagnoses were missed in England. BJU International, 133(5):587-595.
Lüchtenborg, M., Huynh, J., Armes, J., Plugge, E., Hunter, R.M., Visser, R., Taylor, R.M. and Davies, E.A., 2024. Cancer incidence, treatment, and survival in the prison population compared with the general population in England: a population-based, matched cohort study. The Lancet Oncology, 25(5), pp.553-562 https://doi.org/10.1016/S1470-2045(24)00035-4
Miller M, McCann L, Lewis L,Miaskowski C, Ream E, et al. Patients’ and Clinicians’ Perceptions of the Clinical Utility of Predictive Risk Models for Chemotherapy-Related Symptom Management: Qualitative Exploration Using Focus Groups and Interviews. J Med Internet Res 2024;26:e49309 doi: 10.2196/49309
Oakley, C. (2024) How can nurses help patients report neutropenic sepsis? Cancer Nursing Practice. 23, 3, 19. https://doi.org/10.7748/cnp.23.3.19.s8
Varghese, T.S., Andrews, C., Fisher, L., Goldacre, B., Mehrkar, A., Pande, R., Smith, N.A.S., Walker, A.J., Roberts, K.J., Sultana, A., MacKenna, B., Lemanska, A. (2024). Using Data to Improve Healthcare: A Case Study of Pancreatic Enzyme Replacement in Pancreatic Cancer. Seminars in Oncology Nursing, https://doi.org/10.1016/j.soncn.2024.151688
Whitaker, K.L., Perchyk, T., Kerrison, R.S. Lemanska, A. (2024). Challenges in understanding inequities in help-seeking for possible cancer symptoms. BMC Global Public Health 2, 49. https://doi.org/10.1186/s44263-024-00082-1
Aldiss S, Hollis R, Phillips B, et al. (2023) Research priorities for children's cancer: a James Lind Alliance Priority Setting Partnership in the UK. BMJ Open, 13(12), e077387.
Aldiss S, Hart-Spencer P, Langton L, et al. (2023) What matters to you? Engaging with children in the James Lind Alliance Children's Cancer Priority Setting Partnership. Research Involvement and Engagement, 9(1), 110.
Estupiñán Fdez. De Mesa, M., Marcu, A., Ream, E. & Whitaker, K. L. (2023). Relationship between intersectionality and cancer inequalities: a scoping review protocol. BMJ Open, 13, e066637.
Gibson F, Aldiss S (2023) What Are the Consequences of Not Responding to Research Priority Setting Exercises? Cancer Care Research Online 3(1):p e037. DOI: 10.1097/CR9.0000000000000037
Harris, J., Ream, E., Armes, J., Gibson F, Marcu, A., Parsons, C.T, Robinson, A., Varghese, S., Poole, K. (2023). What do we know about the psychosocial issues associated with cancer during pregnancy? A scoping review and gap analysis. BMJ Open, Mar 1;13(3):e063283.
Kerrison, R.S, Gil, N., Travis, E., Jones, R., Whitaker, K.L., Rees, C., Duffy, S., von Wagner, C. (2023) Barriers to Colonoscopy in UK Colorectal Cancer Screening Programmes: Qualitative Interviews with Ethnic Minority Groups, Psycho-Oncology, 32(5):779-792. doi: 10.1002/pon.6123.
Kerrison, R.S, Jones, S., Peng, J., Price, G., Verne, J., Barley, E.A., Lugton, C. (2023) Inequalities in cancer screening participation between adults with and without severe mental illness: results from a cross-sectional analysis of primary care data on English Screening Programmes, British Journal of Cancer, https://doi.org/10.1038/s41416-023-02249-3.
Marcu, A., McGregor, F., Egan, B., Hill, K., Cook, T., & Arber, A. (2023). Developing sustainable patient and public involvement in mesothelioma research: multi-method exploration with researchers, patients, carers, and patient organisations. BMC Research Involvement & Engagement. 9:15.
Morgan, S., Gibson, F., Aldiss, S., Porter, L. (2023) Effective transition of young people with long-term conditions into adult services. Nursing Children and Young People. 35(1), 34–42. https://doi.org/10.7748/ncyp.2022.e1439
Sutton, K., Moore, J., Armes, J., Briggs, E. Perceptions and experiences of the subjective well-being of people with glioblastoma: a longitudinal phenomenological study, Neuro-Oncology Practice 2023. 10: 1, 79 - 88, https://doi.org/10.1093/nop/npac064
Whitaker, K.L., Boswell, L., Russell, J., Black, G.B. Harris, J. The relationship between patient enablement and help-seeking in the context of blood cancer symptoms. Psycho-oncology, DOI: 10.1002/pon.6170
Zasada, M., Harris, J., Groothuizen, J., Aroyewun, E., Mendis, J., Taylor, C., Hewish, M. Investigating the efficiency of lung multi‐disciplinary team meetings—A mixed methods study of eight lung multi‐disciplinary teams. Cancer Medicine. 2023, 12(8):9999-10007. doi: 10.1002/cam4.5730.
Evans, J., Green, D., Connor, G.O., Lanigan, J., Gibson, F. (2022). Nutritional support practices and opinions toward gastrostomy use in pediatric bone marrow transplant centers: A national survey. Nutrition ;95:111556. doi: 10.1016/j.nut.2021.111556.
Faithfull, S., Cockle-Hearne, J., Lemanska, A. et al (2022) Randomised controlled trial to investigate the effectiveness of the symptom management after radiotherapy (SMaRT) group intervention to ameliorate lower urinary tract symptoms in men treated for prostate cancer. Support Care Cancer 30, 3165–3176. https://doi.org/10.1007/s00520-021-06749-x
Forster, A.S, Herbert, A., Koo, M.M., Taylor, R.M., Gibson, F., Whelan, J.S., Lyratzopoulos, G., Fern, L.A. (2022). Associations between diagnostic time intervals and health-related quality of life, clinical anxiety and depression in adolescents and young adults with cancer: cross-sectional analysis of the BRIGHTLIGHT cohort. British Journal of Cancer, doi: 10.1038/s41416-022-01698-6.
Gordon, R., Fawson, S., Moss‐Morris, R., Armes, J. and Hirsch, C.R., 2022. An experimental study to identify key psychological mechanisms that promote and predict resilience in the aftermath of treatment for breast cancer. Psycho‐Oncology, 31(2), pp.198-206. doi:10.1002/pon.5806
Hudson, L.D., Chapman, S., Street, K.N., Nicholls, D., Roland, D., Dubicka, B., Gibson, F., Mathews, G., Viner, R.M (2022). Increased admissions to paediatric wards with a primary mental health diagnosis: results of a survey of a network of eating disorder paediatricians in England. Archives of Diseases in Childhood;107(3):309-310. doi: 10.1136/archdischild-2021-322700.
Ip, A., Black, G., Vindrola-Padros, C., Taylor, C., Otter, S., Hewish, M., Bhuiya, A., Callin, J., Wong, A., Machesney., Fulop, N., Taylor, C., Whitaker, K.L. (2022). Socioeconomic differences in help-seeking experiences in primary care for symptoms related to colorectal cancer during COVID-19: A UK-wide qualitative interview study. British Journal of General Practice, https://bjgp.org/content/early/2022/03/24/BJGP.2021.0644
Lea, S., Taylor, R., Gibson, F. (2022). Developing, nurturing, and sustaining an adolescent and young adult-centered culture of care. Qualitative Health Research DOI: 10.1177/10497323221084910
Lemanska, A., Poole, K., Manders, R. et al (2022). Patient activation and patient-reported outcomes of men from a community pharmacy lifestyle intervention after prostate cancer treatment. Support Care Cancer 30, 347–358, https://doi.org/10.1007/s00520-021-06404-5
Oulton, K., Wray, J., Kelly, P., Khair, K., Sell, D., Gibson, F (2022). Culture, cognisance, capacity and capability: The interrelationship of individual and organisational factors in developing a research hospital. Journal of Clinical Nursing. ;31:362– 377. https://doi.org/10.1111/jocn.15867
Patel, V., Kerrison, R.S. (2022) Patients’ and physicians’ experiences with remote consultations in primary care, during the covid-19 pandemic: a multi-method rapid review of the literature. BJGP Open, https://bjgpopen.org/content/early/2022/04/14/BJGPO.2021.0192
Sipanoun, P., Oulton, K., Gibson, F., Wray, J (2022). The experiences and perceptions of users of an electronic patient record system in a pediatric hospital setting: a systematic review. International Journal of Medical Informatics. 19;160:104691. doi: 10.1016/j.ijmedinf.2022.104691.
Tanay, M. A. L., Armes, J., Oakley, C., Bryson, L., Johnston, R., Moss-Morris, R., Rafferty, A. M., Roca, J., Sage, L., Tanner, D., Urwin, L., Wyatt, T., & Robert, G. (2022). Co-designing a behavioural intervention for reducing the impact of chemotherapy-induced peripheral neuropathy symptoms: An evidence- and theory-driven approach. European Journal of Cancer Care, e13671. https://doi.org/10.1111/ecc.13671
Tanay, M.A.L., Armes, J., Oakley, C. et al. Co-designing a cancer care intervention: reflections of participants and a doctoral researcher on roles and contributions. Res Involv Engagem 8, 36 (2022). https://doi.org/10.1186/s40900-022-00373-7
van Os, S., Syversen, A., Whitaker, K.L., Quaife, S.L., Janes, S.M., Jallow, M., Black, G (2022). Lung cancer symptom appraisal, help-seeking and diagnosis - rapid systematic review of differences between patients with and without a smoking history. Psychooncology.;31(4):562-576. doi: 10.1002/pon.5846.
Bryan, G., Kelly, P., Chesters, H. Franklin, J. Griffiths, H. Langton, L. Langton, L. Wakefield, CE. Gibson, F (2021). Access to and experience of education for children and adolescents with cancer: a scoping review protocol. Systematic Reviews 10, 167
Byrne, J.V., Whitaker, K.L., Black, G.B (2021). How doctors make themselves understood in primary care consultations: A mixed methods analysis of video data applying health literacy universal precautions. PLoS One. 21;16(9):e0257312. doi: 10.1371/journal.pone.0257312.
Cockle-Hearne, J., Aldiss, S., Gibson, F., Milne, S., Todd, J., Ream, E. (2021). Support interventions provided during palliative care to families with dependent children when a parent has terminal illness: a scoping review protocol. JBI Evidence Synthesis. 2021 Jun 7;19(11):3163-3173. doi: 10.11124/JBIES-20-00472.
Courtier, N,, Armes, J., Smith, A., Radley, L., Hopkinson, J.B (2021). Targeted self-management limits fatigue for women undergoing radiotherapy for early breast cancer: results from the ACTIVE randomised feasibility trial. Support Care Cancer, doi: 10.1007/s00520-021-06360-0.
Faithfull, S., Lemanska, A., Poole, K., Aning, J., Manders, R., et al (2021). Obesity and low levels of physical activity impact on cardiopulmonary fitness in older men after treatment for prostate cancer. European Journal of Cancer Care, 30( 6), e13476. https://doi.org/10.1111/ecc.13476
Gibson, F., Fern, L.A., Phillips, B., Gravestock, H., Malik, S., Callaghan, A., et al (2021). Reporting the whole story: Analysis of the 'out-of-scope' questions from the James Lind Alliance Teenage and Young Adult Cancer Priority Setting Partnership Survey. Health Expectations;24(5):1593-1606. doi: 10.1111/hex.13276.
Gordon, R., Fawson, S., Moss-Morris, R., Armes, J., Hirsch, C.R (2021). An experimental study to identify key psychological mechanisms that promote and predict resilience in the aftermath of treatment for breast cancer. Psychooncology. 2021; 1- 9. doi:10.1002/pon.5806
Maguire, R., McCann, L., Kotronoulas, G., Kearney, N., Ream, E., Armes, J. et al (2021). Real time remote symptom monitoring during chemotherapy for cancer: European multicentre randomised controlled trial (eSMART) BMJ; 374 :n1647 doi:10.1136/bmj.n1647
Morgan, J., Evans, C., Beresford, L., Bryan, G., Fulbright, H., Phillips, B (2021). A systematic review of early phase studies for children and young people with relapsed and refractory rhabdomyosarcoma. PROSPERO 2021 CRD42021266254 https://www.crd.york.ac.uk/prospero/display_record.php?ID=CRD4202126625….
Quinn-Scoggins, H.D., Cannings-John, R., Moriarty, Y., Whitelock, V., Whitaker, K.L., Grozeva, D., et al (2021). Cancer symptom experience and help-seeking behaviour during the COVID-19 pandemic in the UK: a cross-sectional population survey, BMJ Open, doi: 10.1136/bmjopen-2021-053095
Ream, E., Richardson, A., Lucas, G., Marcu, A., Foster, R., Fuller, G., Oakley, C. (2021). Understanding the support needs of family members of people undergoing chemotherapy: A longitudinal qualitative study. European Journal of Oncology Nursing, 50, 101861. https://doi.org/10.1016/j.ejon.2020.101861
Slade, A., Retzer, A., Ahmed, K., Kyte, D., Keeley, T., Armes, J., Brown, J. Calman, L., Gavin, A., Glaser, A., Greenfield, D., Lanceley, A., Taylor, R., Velikova, G., Turner, G., Calvert, M (2021). Review of the Use of Translated Patient Reported Outcome Measures in Cancer Trials. Trials 22, 306. https://doi.org/10.1186/s13063-021-05255-z
Tanay, M.A., Armes, J., Moss-Morris, R., Rafferty, A.M. & Robert, G (2021). A systematic review of behavioural and exercise interventions for the prevention and management of chemotherapy-induced peripheral neuropathy symptoms. Journal of Cancer Survivorship. https://doi.org/10.1007/s11764-021-00997-w
Tanay, M.A., Robert, G., Rafferty, A. M., Moss-Morris, R., & Armes, J. (2021). Clinician and patient experiences when providing and receiving information and support for managing chemotherapy-induced peripheral neuropathy: a qualitative multiple methods study. European Journal of Cancer Care. https://doi.org/10.1111/ecc.13517
Taylor, C., Harris, J., Stenner, K., Sevdalis, N. and Green, S.A.J. (2021),. Cancer Medicine. https://doi.org/10.1002/cam4.3719
Visser, R., Barber, AE., X, A., Mullen P. & Armes, J. (2021). Collaboration with people with lived experience of prison: reflections on researching cancer care in custodial settings. Research Involvement & Engagement 7, 48. https://doi.org/10.1186/s40900-021-00284-z
Archer, S., Holch, P., Armes, J., Calman, L., Foster, C., Gelcich, S., MacLennan, S. & Absolom, K. (2020) ‘No turning back’ Psycho-oncology in the time of COVID-19: Insights from a survey of UK professionals. Psycho-Oncology https://doi.org/10.1002/pon.5465
Cheevers, K., Armes, J., Harris, J. & Rafferty, A.M. (2020). Adaptation and preliminary testing of the registered nursing forecasting (RN4CAST) nurse survey for use in the ambulatory chemotherapy setting. European Journal of Oncology Nursing, 47:101794
Cheng, K.K-F., Siah, R.C-J., Ream, E., Kanesvaran, R., & Armes J. (2020). Protocol for a scoping review of digital health for older adults with cancer and their families. BMJ Open 10:e038876.doi: http://dx.doi.org/10.1136/bmjopen-2020-038876
Cockle-Hearne, J., Reed, E., Todd, J., Ream, E. (2020). The dying parent and dependent children: a nationwide survey of hospice and community palliative care support services. BMJ Supportive & Palliative Care. 2020;bmjspcare-2019-001947. doi:10.1136/bmjspcare-2019-001947
Green, R. (2020). The Forms and Uses of Acquired Prostate Cancer Expertise Among Prostate Cancer Survivors. Sociological Research Online. doi:10.1177/1360780420905840
Hannaford, P.C., Thornton, A.J, Murchie, P., Whitaker, K.L., Adam, R., et al. (2020) Patterns of symptoms possibly indicative of cancer and associated help-seeking behaviour in a large sample of United Kingdom residents—The USEFUL study. PLOS ONE 15(1): e0228033. https://doi.org/10.1371/journal.pone.0228033
Jones,D., Neal R.D., Duffy, S.R.G., Scott, S. E., Whitaker, K.L, Brain,K. (2020) Impact of the COVID-19 pandemic on the symptomatic diagnosis of cancer: the view from primary care. Lancet Oncology, doi: 10.1016/S1470-2045(20)30242-4
Koo, M.M., Lyratzopoulos, G., Herbert, A., Abel, G.A., Taylor, R.M. Barber, J.A., Gibson, F., Whelan, J., Fern, L.A. (2020) Association of self-reported presenting symptoms and timeliness of help-seeking among adolescents and young adults with cancer. JAMA Network Open. 2020;3(9):e2015437. doi:10.1001/jamanetworkopen.2020.15437
Lemanska, A., Byford, R.C., Cruickshank,C., Dearnaley, D.P., Ferreira, F., Griffin, C., Hall, E., Hinton, W., de Lusignan, S., Sherlock, J., Faithfull, S. (2020) Linkage of the CHHiP randomised controlled trial with primary care data. A study investigating ways of supplementing cancer trials and improving evidence-based practice. BMC Medical Research Methodology, doi: 10.1186/s12874-020-01078-9
McHale, C.T., Cruickshank, S., Torrens, C., Armes, J., Fenlon, D., Banks, E., Kelsey, T. and Humphris, G.M., (2020). A controlled pilot trial of a nurse-led intervention (Mini-AFTERc) to manage fear of cancer recurrence in patients affected by breast cancer. Pilot and Feasibility Studies, 6,1, 60. https://doi.org/10.1186/s40814-020-00610-4
Pearce, S., Gibson, F., Whelan, J., Kelly, D. (2020) Untellable tales and uncertain futures: the unfolding narratives of young adults with cancer. International Journal of Social Research Methodology, 23 (4), 377-390
Ream, E., Hughes, A.E., Cox, A., Skarparis, K., Richardson, A., Pedersen, V.H, Wiseman, T., Forbes, A., Bryant, A (2020. Telephone interventions for symptom management in adults with cancer. Cochrane Database of Systematic Reviews, Issue 6. doi: 10.1002/14651858.CD007568.pub2.
Taylor, R.M., Lobel, B., Thompson, K., Onashile, A., Croasdale, M., Hall, N., Gibson, F., Martins, A., Wright, D., Morgan, S., Whelan, J.S., Fern, L.A. (2020) BRIGHTLIGHT researchers as ‘dramaturgs: creating There is a Light from complex research data. Research Involvement and Engagement. 6: 48. 10. doi: 10.1186/s40900-020-00222-5
Aldiss, S., Fern, L.A., Phillips, B., Callaghan, A., Dyker, K., Gravestock, H., Groszmann, M., Hamrang, L., Hough, R., McGeachy, D., Morgan, S., Smith, S., Upadhyaya, S., Veitch, H., Veitch, L., Williamson, M., Whelan, J., Gibson, F. (2019) Research priorities for young people with cancer: a UK priority setting partnership with the James Lind Alliance. BMJ Open, 9(8):e028119.
Aldiss, S., Rose, L., McCutcheon, D., Cass, H., Ellis, J., Gibson, F. (2019) Gathering expert opinion to inform benchmarks to support transitional care. Journal of Child Health Care, 23(1):131-146.
Amelung, D., Whitaker, K.L, (joint first author), Lennard, D., Ogden, M., Sheringham, J., Zhou, Y., Walter, F.M., Singh, H., Vincent, C., Black G. (2019) The influence of doctor-patient conversations on behaviours of patients presenting to primary care with new or persistent symptoms: A video observation study. BMJ Quality Safety, doi.org/10.1136/bmjqs-2019-009485.
Bryan, G., Bluebond-Langner, M., Kelly, D., Kumpunen, S., Oulton, K., Gibson, F. (2019) Studying children’s experiences in interactions with clinicians: identifying methods fit for purpose. Qualitative Health Research, 29 (3): 393-403
Franklin, P., Arber, A., Reed, L. Ream, E. (2019) Health and social care professionals’ experiences of supporting parents and their dependent children during, and following, the death of a parent: A qualitative review and thematic synthesis, Palliative Medicine, 33(1), pp.49-65.
Kyte, D., Retzer, A., Ahmed, K., Keeley, T., Armes, J., Brown, J.M., Calman, L., Gavin, A., Glaser, A.W., Greenfield, D.M., Lanceley, A., Taylor, R.M., Velikova, G,. Michael D. Brundage., Efficace, F., Mercieca-Bebber, R., King, M.T., Turner, G., Calvert, M. (2019) Systematic evaluation of Patient-Reported Outcome protocol content and reporting in cancer trials, JNCI: Journal of the National Cancer Institute, jz038, doi.org/10.1093/jnci/djz038
Lea, S., Gibson, F., Taylor, R.M. (2019) The culture of young people's cancer care: A narrative review and synthesis of the UK literature. European Journal of Cancer Care 28 (3):e13099 doi.org/10.1111/ecc.13099
Lemanska, A., Poole, K., Griffin, B., Manders, R., Saxton, J.M., Turner, L., Wainwright, J., Faithfull, S. (2019) Community pharmacy lifestyle intervention to increase physical activity and improve cardiovascular health of men with prostate cancer: a phase II feasibility study, BMJ Open 9 (6) e025114 DOI: 10.1136/bmjopen-2018-025114
Marcu, A., Muller, C., Ream, E., Whitaker, K.L. (2019). Online information-seeking about potential breast cancer symptoms: Capturing online behaviour with an internet browsing tracking tool. Journal of Medical Internet Research, 21, e12400, doi.org/10.2196/12400.
Martin Payo, R., Harris, J., Armes, J. (2019) Prescribing fitness apps for people with cancer: a preliminary assessment of content and quality of commercially available apps, Journal of Cancer Survivorship, doi.org/10.1007/s11764-019-00760-2
Pearce. S., Whelan, J., Kelly, D., Gibson, F. (2019) Renegotiation of identity in young adults with cancer: a longitudinal narrative study. International Journal of Nursing Studies 102, 103465
Poole K., Ogden J., Gasson S., Lemanska A., Archer F., Griffin B., Saxton J., Lyons K. and Faithfull S. (2019) Creating a teachable moment in community pharmacy for men with prostate cancer: A qualitative study of lifestyle changes. Psycho-Oncology, doi.org/10.1002/pon.4983
Skrobanski, H., Ream, E., Poole, K., Whitaker, K.L. (2019) Understanding primary care nurses’ contribution to cancer early diagnosis: A systematic review. European Journal of Oncology Nursing, 41, 149-164, doi.org/10.1016/j.ejon.2019.06.007
Research Group members
Expert Group leads

Professor Katriina Whitaker
Professor of Psychology and Co-Lead for Cancer Care

Dr Robert Kerrison
Associate Professor and Co-Lead for Cancer Care
Expert Group members

Susie Aldiss
Research Fellow (Child Health)

Dr Anne Arber
Visiting Reader in Cancer and Palliative Care

Professor Jo Armes
Professor of Cancer Care and Lead for Digital Health

Dr David Bartlett
Senior Lecturer of Exercise Immunology

Laura Boswell
Postgraduate Researcher

David Brighton
Lecturer, (adult nursing)

Dr Gemma Bryan
Senior Research Fellow

Hugh Claridge
Postgraduate Research Student

Zoe Clothier
Research Assistant

Dr Jane Cockle Hearne
Research Fellow

Dr Anna Cox
Senior Lecturer in Health and Social Care

Dr Christos Dadousis
Research Fellow in Health and Biomedical Informatics Research Group
Mar Estupiñan Fernandez De Mesa
Fellow in Cancer Care

Professor Faith Gibson
Professor of Child Health and Cancer Care

Natalie Gil
Postgraduate Researcher

Dr Jenny Harris
Senior Lecturer in Cancer Care and Health Statistics

Esra Hassan
Research Fellow

Dr Chris Jacobs
Associate Professor, Genetic and Genomic Counselling, Interim Associate Head Research & Innovation, School of Health Sciences

Dr Robert Kerrison
Associate Professor and Co-Lead for Cancer Care
Dr Afrodita Marcu
Research Fellow (RA II)

Jackie McBride
Associate Head of School – Education

Sophie McGrevey
Research Assistant

Lizzie Merrill
Research Fellow in Cancer Care

Tetyana Perchyk
Research Fellow in Health Data Science

Claire Price
Postgraduate Research Student

Alexandra Pritchard
Postgraduate Research Student

Professor Emma Ream
Professor, Director of Health Sciences Research

Dr Katie Sutton
Research Fellow
Related sustainable development goals